Understanding Superficial Venous Reflux
Superficial venous reflux develops when the valves of a vein become damaged and/or diseased. In venous insufficiency states, venous blood escapes from its normal upward path of flow and refluxes backward down the veins into an already congested leg. Venous insufficiency syndromes are caused by valvular incompetence in the high-pressure deep venous system, low-pressure superficial venous system, or both. Valves may fail, causing insufficiency, for a variety of reasons. Failures over time can cause veins to become dilated and tortuous, and are eventually recognized as varicose veins. Untreated venous insufficiency in the deep or superficial system causes a progressive syndrome involving pain, swelling, skin changes, and eventual tissue breakdown.
Symptoms of Venous Reflux Disease
Symptoms of venous reflux disease can include aching, burning, swelling, itching, unsightly cosmetic appearance, skin discoloration and ulcers. (Examples below)
Skin Dermatitis
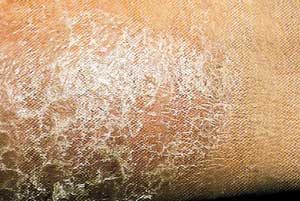
Foot Edema
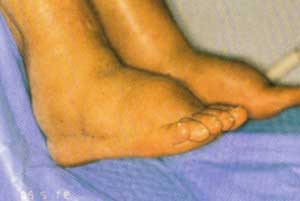
Vallux Bleeder
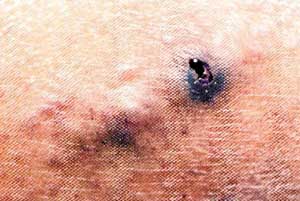
Venous Ulcer
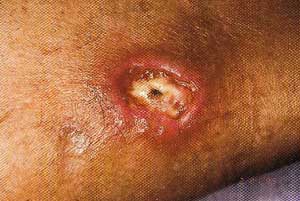
Understanding Superficial Venous Reflux
Superficial venous reflux develops when the valves of a vein become damaged and/or diseased. In venous insufficiency states, venous blood escapes from its normal upward path of flow and refluxes backward down the veins into an already congested leg. Venous insufficiency syndromes are caused by valvular incompetence in the high-pressure deep venous system, low-pressure superficial venous system, or both. Valves may fail, causing insufficiency, for a variety of reasons. Failures over time can cause veins to become dilated and tortuous, and are eventually recognized as varicose veins. Untreated venous insufficiency in the deep or superficial system causes a progressive syndrome involving pain, swelling, skin changes, and eventual tissue breakdown.
Symptoms of Venous Reflux Disease
Symptoms of venous reflux disease can include aching, burning, swelling, itching, unsightly cosmetic appearance, skin discoloration and ulcers. (Examples below)
Skin Dermatitis

Foot Edema

Vallux Bleeder

Venous Ulcer







